An invitation to see the interconnected embodied whole.
Interested in our initiative? Submit your email to receive an invite to the alive collective.
Menu
Interested in our initiative? Submit your email to receive an invite to the alive collective.
An invitation to see the interconnected embodied whole.

Written by Johanna Lynch – University of Queensland
As I write the first of a series of articles for the ALIVE Writer-in-Residence program I am wrestling with where to start and how to talk in a series of separate articles about the interconnected wonderfulness of being a whole complex person. My solution is to plan a series that reflects on the interconnections of facets of being whole. Over this set of essays, we will reflect together on being whole people who sense, feel, experience, connect, comfort, defend, encourage, and heal. These themes are intentionally verbs, not nouns. They describe active processes that we can all be part of for our own wholeness and to help us see the wholeness of others.
As some of you may know, I am an Australian General Practitioner (GP) who became a GP psychotherapist so I could care for people that the mental health services in my community dismissed, ignored, or pathologised. I have become fascinated and passionate about making sure that whole person care becomes normal care in health, education, and the social services sector. This has led me on a journey of learning about trauma, grief, attachment, and the biology of stress (and so much more across the disciplines). At one point (2009- 2013) it led me to create a transdisciplinary clinic called Integrate Place that offered generalist care, art therapy, trauma-informed yoga, mental health nursing, and attachment based social work care to adults who had survived trauma and neglect in their community.
This passion for whole person care also led me to research. It led me to reflect on the philosophy of how we know about people and how people change and grow. It also made me search for shared language and goals that might unify how the disciplines see and care for whole complex people This search led me to see how biotechnical approaches that highly value precision and prediction have an inbuilt narrowed gaze that blinds them to the rich complexity of how culture, relationships, meaning and context impact health. It also made me fall back in love with generalism – a way of seeing, listening, questioning, discerning, and caring that integrates both the biography and biology of each person as part of a complex whole. 1p.5,2-5
In this series of essays, we will reflect on ways of seeing and being and knowing that help us to see whole people. We will start with the verb sensing. What do you think of when you think of the word sensing?
For me as a clinician indoctrinated in the value of a certain kind of ‘evidence’, the word sensing used to imply something unreliable, not precise or predictive enough to be useful for medical decision making, and perhaps the worst accusation: ‘anecdotal’ which was code for ‘unscientific’. This suspicion was applied to both the patient’s sensations and the clinician’s own invisible internal praxis wisdom and intuition. Sensing was often described in medical settings as ‘subjective’ – a kind of dismissive reductionist code for ‘not objective’ or even ‘not real’. We sometimes see this in descriptions of symptoms as ‘psychological’ or the slightly less offensive ‘functional’ (implying subjective, internal, invisible but impacting someone’s capacity to function) compared to ‘organic’ (implying observable, objective, or real to the clinician). But is it reliable and scientific to only value as ‘real’ what can be observed from outside?
Meanwhile, over the years, I have been learning from the brave honesty of the people I cared for as they described their life stories, inner experiences, memories, yearning, pains, and joys. Their insightful and reasoned reflections on their lived experience have changed me. Miranda Fricker says it is unjust to not value knowledge from inside the knower.6 Inner subjective knowledge requires different ways of understanding that are not focussed on precision and prediction. To see internal processes, we need to value knowledge that is experiential, authentic, culturally grounded, meaning making, and created with other people in relationship. This way of knowing adds so much to how we understand the world.
In a world obsessed by ‘science’ as ‘reality’, it is perhaps important to notice that subjective information is also ‘scientific’ – if we agree with Iain McGilchrist’s definition of science as: “neither more nor less than patient detailed attention to the world”. 7p.5 Sensing is not just ‘anecdote’; it is a complex experiential way of knowing.
It is also important to critique the archaic assumptions of those who overvalue objectivity and assume that the body is an object that is ‘completely explorable’.8p.2 Assumptions that the disembodied observer’s (‘objective’) mind is more reasonable and reliable than their own subjective experience (or that of the person they are caring for) are not aligned with the current science of a complex interconnected person.9
This brings us back to sensing. I have become completely fascinated by how sensing is an interconnected continuous oscillatory feedback process between inner and outer knowing.10,11 Sensing is not just a simple linear process of perceiving, thinking and acting. For example, the sensors in the microbiome unconsciously influence mood, and past experience can alter our perception. Each time we sense something in our inner or outer worlds, our conscious and unconscious awareness links to our life story, beliefs, reasoning, and intuition as we ‘make-sense’ of the world.
Sensing is so complex and interconnected that it completely blows apart any artificial distinctions between objective and subjective, body and mind, inner and outer, and even past and present.
I have come to love sensation as a kind of moment-by-moment way of knowing about the world that integrates and connects the whole, and is owned by the knower. Only they can know what they sense, it cannot be defined from outside. Sensing and sense-making are so intertwined.12,13 Sensing is a kind of unity, a perception of the whole, not just a bodily reaction to environment.
Along with new understanding of the multilayered whole person, there is a growing literature that explores the role of a part of the brain called the insula. The insula organises, connects,14 interprets14,15 and integrates sensation, perception, emotion, thoughts and plans. Florian Kurth says this creates “one subjective image of ‘our world’.”16p.519 Although this image is not always accurate, or complete, or conscious, it matters.
Interestingly, when people are asked to rate their own health, their sense is more accurate than medical assessments of their wellbeing. Marja Jylha calls self-rated health a “cross-road between the social world and psychological experiences on the one hand and the biological world on the other.”17p.308 This cross-road is where those who offer whole person care need to sit, listen, learn, and care. Respect for sensing could help us all, in Bradley Lewis’s words, to develop “better, truer, richer, and more generous stories … in the service of healing and coping.18p.196
Sensation is also responsive to small changes, tuned in to relationships, context, inner values and history. Our cells sense danger, and temperature change and oxygen levels (and so much more!). We sense ourselves in relationship to gravity and movement (proprioception), and the circadian rhythms of the sun. We even sense what is behind us. We use our senses to relate to others – to tune into their facial expressions and tone of voice (known as prosody). When we are fearful, we find it harder to hear the human voice as our ear drum changes to hear low sounds. We sense our emotions, and we sense threat (what Stephen Porges has called ‘neuroception’19), and we sense our capacity to cope. We sense when we belong, and whether we have existential or spiritual peace or despair. We even sense our relationship to place (connection to country) and to the future (sense of hope).
As you are reading this – I am wondering if you could reflect on your current ‘sense of’ yourself? Where are you and who is nearby? How do you sense yourself and your spirit? When you tune into it are you aware of interconnections and how you know about your whole person?
When all these layers of sensation work seamlessly together, they often go unnoticed, and yet they have a purpose: to help us to enjoy and be safe in our world. In my doctoral research exploring threat and sense of safety,3 it emerged that sensation protects our:
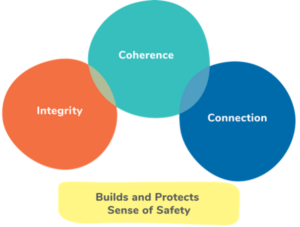
Figure 1: What senses protect: From the cellular to the communal
(Used with permission Figure 5.1 Lynch, J.M. (2021) A whole person
approach to wellbeing: Sense of safety. Routledge: UK (p.78)
In complex systems, reality is probed, sensed and responded to.20 So if we want to know about complex whole people, we need to value and respect sensation. We also need to understand its limitations, the way it can be numbed, or dissociated, or hyperaware and hypervigilant, or distorted, altered, and confusing.
Awareness of sensation and sense-making can transform clinical practice. In my work with adult survivors of childhood maltreatment, I had to learn to be very aware of sensation – my own and those of the person I was caring for. Sensation became a friend as it prioritised the voice of the person who was sensing, and reduced the focus on what Paul Verhaeghe critiques as the ‘ascendant medical observer’.21 Sensing was also a gift through grounding techniques, attuned therapeutic connection, and learning to trust my own intuitions. It became a guide when trying to understand something embodied that had no words in assessment and in my own selfcare. It also helped me to make sense of coping mechanisms: how disconnection, numbness, distraction (for example using obsessions and addictions), or creative flow and activity helped people to alter their sensations to a dose they could tolerate.
Sensing became a way to understand whole people. Rather than being dismissed as anecdotal evidence, it is now central to both assessment and treatment. Sensing can help both people in the therapeutic relationship to tune into their own needs. Highlighting a person’s ‘sense of…’ is an amazing combination of subjective and objective knowing that normalises caring for the many layers of being a whole person. Understanding the beautiful complexity of sensing could transform care.
References
About the writer

Dr Johanna Lynch MBBS PhD FRACGP FASPM Grad Cert (Grief and Loss) is a retired GP who writes, researches, teaches, mentors and advocates for generalist and transdisciplinary approaches to distress that value complex whole person care and build sense of safety. She is an Immediate Past President and Advisor to the Australian Society for Psychological Medicine and is a Senior Lecturer with The University of Queensland’s General Practice Clinical Unit. She spent the last 15 years of her 25 year career as a GP caring for adults who are survivors of childhood trauma and neglect. She consults to a national pilot supporting primary care to respond to domestic violence.
An invitation to resist ignoring invisible causes of suffering and strength.
Read moreAn invitation to consider the links between wholeness and healing.
Read moreCongratulations to Rebecca Moran and team from the Big Anxiety Research Centre for TheMHS 2024 Lived Experience Led Storytelling Award!
Read moreAn invitation to consider the biology of belonging.
Read moreAn invitation to see social determinants of health in a new light.
Read moreAn invitation to critique current understanding of mood as disorder.
Read moreAn invitation to see the interconnected embodied whole.
Read moreby Next Generation Researcher Network
Read moreApplications closed for 2024 round
Read moreCongratulations to this year’s awardees and stay tuned for the next call out!
Read moreA Call to Action to [Re]form National Mental Health and Well-Being, March 2024
The ALIVE National Centre Next Generation Researcher Network Capacity Building Funding Scheme 2024
Read moreTo address capabilities needs, career pathways, conditions in research organisations and identify lived-experience approaches and practices for research integration
Read moreThis handbook has been co-designed by members of the Co-Design Living Labs Network.
Find out more about the noticeboard feature and how to contribute
Read moreA capacity building and career development initiative of the ALIVE National Centre for Mental Health Research Translation
Read moreThis is a monthly event focused on bringing people together to discuss and translate the findings in mental health research.
The ALIVE National Centre is funded by the NHMRC Special Initiative in Mental Health.
The ALIVE National Centre for Mental Health Research Translation acknowledges the Traditional Owners of the land on which we work, and pay our respects to the Elders, past and present. We are committed to working together to address the health inequities within our Aboriginal and Torres Strait Islander communities.
WARNING: Aboriginal and Torres Strait Islander viewers are warned that this site may contain images and voices of deceased persons.
This map attempts to represent the language, social or nation groups of Aboriginal Australia. It shows only the general locations of larger groupings of people which may include clans, dialects or individual languages in a group. It used published resources from the eighteenth century-1994 and is not intended to be exact, nor the boundaries fixed. It is not suitable for native title or other land claims. David R Horton (creator), © AIATSIS, 1996. No reproduction without permission. To purchase a print version visit: https://shop.aiatsis.gov.au/



The ALIVE National Centre for Mental Health Research Translation is funded by the National Health and Medical Research Council (NHMRC) Special Initiative in Mental Health GNT2002047.
ALIVE Next Generation Researcher Network Application Form Click here
For University based research higher degree students, early/mid-career mental health researchers
ALIVE Lived Experience Research Collective Application Form Click here
For University and community based lived-experience or carer-focused mental health researchers at all career stages
ALIVE Collective Application Form Click here
For any individuals or organisations with a general interest in supporting the special initiative in mental health
ALIVE Implementation and Translation Network (ITN) Application Form Click here
For sector, service delivery organisations in mental health serving people across the life course and priority populations
If you have a general enquiry about The Alive National Centre for Mental Health Research Translation, please submit an enquiry below
Not a member of the ALIVE National Centre? Register now
ALIVE Next Generation Researcher Network Application Form Click here
For University based research higher degree students, early/mid-career mental health researchers
ALIVE Lived Experience Research Collective Application Form Click here
For University and community based lived-experience or carer-focused mental health researchers at all career stages
ALIVE Collective Application Form Click here
For any individuals or organisations with a general interest in supporting the special initiative in mental health
ALIVE Implementation and Translation Network (ITN) Application Form Click here
For sector, service delivery organisations in mental health serving people across the life course and priority populations
If you have a general enquiry about The Alive National Centre for Mental Health Research Translation, please submit an enquiry below